Peripheral angioplasty is a minimally invasive medical procedure aimed at treating peripheral artery disease (PAD), a common circulatory problem where narrowed arteries reduce blood flow to your limbs. PAD typically affects the legs, but can also damage arteries in the kidneys, arms, stomach, and head. This comprehensive blog post delves into the essentials of peripheral angioplasty, including its purpose, procedure, benefits, risks, and recovery.
Understanding Peripheral Angioplasty
Peripheral angioplasty is often recommended when PAD causes significant pain or interferes with daily activities. The main goals are to improve blood flow in the affected peripheral artery, relieve symptoms, enhance mobility, and prevent the risk of heart attacks, strokes, or limb amputation.
The Procedure
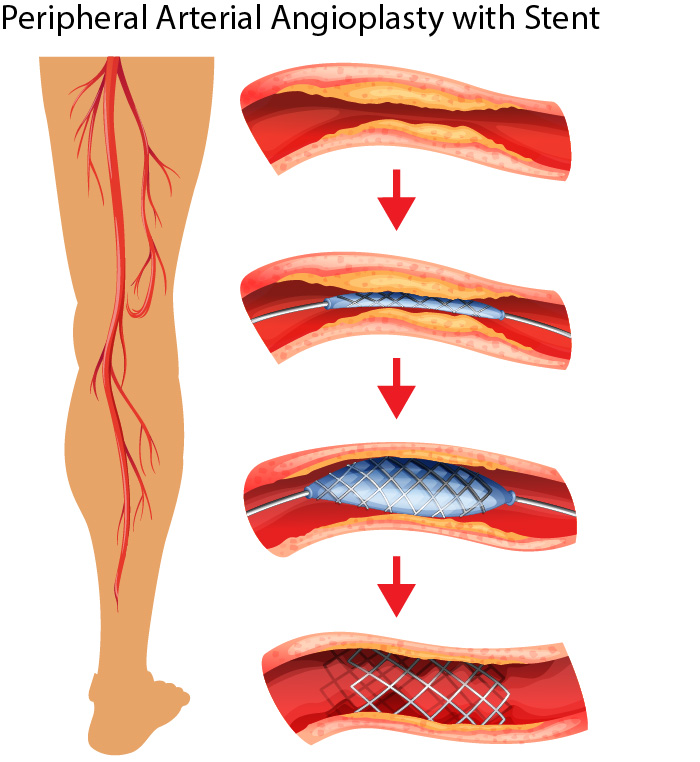
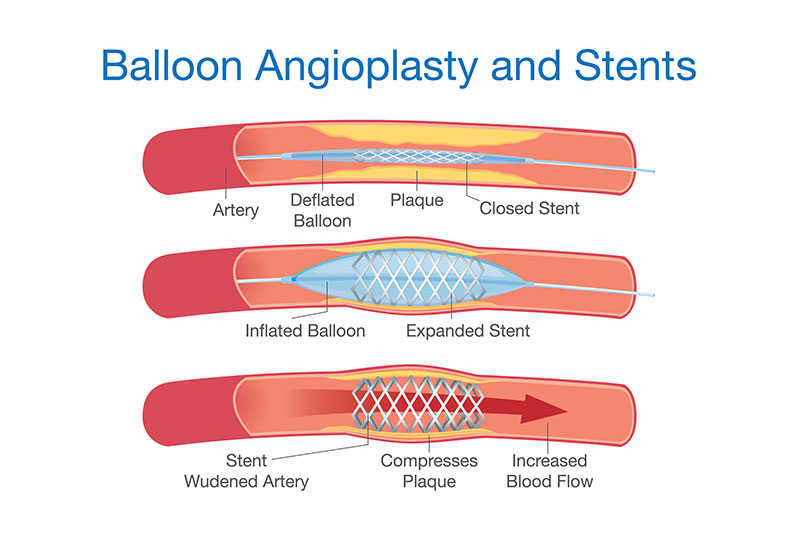
Peripheral angioplasty involves the use of a catheter (a thin, flexible tube) that is threaded through a blood vessel to the site of the narrowed or blocked artery. The catheter has a small inflatable balloon at its tip. Once in place, the balloon is inflated to widen the artery, improving blood flow. In some cases, a stent (a small, wire mesh tube) is placed in the artery to keep it open.
The procedure is typically performed under local anesthesia and may require a short hospital stay. Advances in technology and technique have made it safer and more effective over the years.
Benefits
The primary benefit of peripheral angioplasty is the improvement in blood flow and the reduction or elimination of PAD symptoms such as leg pain, cramping, and fatigue, especially during physical activities. Patients often experience a significant improvement in their quality of life, with increased mobility and reduced risk of serious complications associated with PAD.
Risks
As with any medical procedure, peripheral angioplasty carries some risks, though they are relatively low. These may include reactions to the contrast dye, bleeding at the catheter insertion site, infection, artery damage, and in rare cases, the need for emergency bypass surgery if the procedure is not successful. The risk of complications is higher in individuals who have diabetes, chronic kidney disease, or those who smoke.
Recovery
Recovery from peripheral angioplasty usually involves a short hospital stay followed by a period of rest at home.

Conclusion
Peripheral angioplasty has emerged as a key intervention for managing peripheral artery disease, offering patients relief from symptoms and a path towards a more active lifestyle. While it is not a cure for PAD, it significantly improves quality of life for many patients. It’s important for individuals undergoing this procedure to adopt healthy lifestyle changes, such as quitting smoking, eating a balanced diet, and exercising regularly, to ensure the long-term success of the treatment and to prevent the progression of the disease. Collaboration between healthcare providers and patients in managing PAD through peripheral angioplasty and lifestyle adjustments can lead to the best outcomes, enhancing both longevity and quality of life.
Our Doctors
Dedicated IR Center for Vascular Problems in Madhya Pradesh
DR. SHAILESH GUPTA
MD, PDCC (INTERVENTIONAL RADIOLOGY) Consultant & Co-Director CVIC (Center Of Vascular & Interventional Care)
DR. ALOK KUMAR UDIYA
MD Radiology, PDCC (Neurointervention Radiology), PDCC ( HPB Intervention Radiology) FINR (Switzerland) & EBIR
Endovascular Surgeon & Consultant Interventional Neuroradiologist at Care CHL Hospital, Indore Co-director CVIC( center for vascular and interventional care)https://interventionradiologyindore.com/
DR. NISHANT BHARGAVA
Consultant Intervention Radiologist
MD Radiology, PDCC ( Neurointervention Radiology), FINR ( Fellowship in Neurointervention Radiology)
Co-director CVIC(Center for Vascular and Interventional Care)
Contact Details
Phone no.
0731 4675670
+91 9827760073
Facebook
https://www.facebook.com/profile.php?id=100092538633553&mibextid=ZbWKwL
Instagram
https://instagram.com/cvic_center?igshid=ZGUzMzM3NWJiOQ==
Google My business
https://g.co/kgs/DrdV3T
YouTube
https://www.youtube.com/channel/UCP5TH5e4iQZkpDUgnLsgZhw
Pinterest
https://pin.it/5DzpX5Z
Twitter
https://x.com/cviccenter?t=01TclSrLFdu0K2re0Gs96w&s=08
LINKEDIN
https://www.linkedin.com/company/center-of-vascular-interventional-care/
Location
Read More –
Mechanical Thrombectomy for acute stroke in Neuro Intervention – https://cvicvascular.com/mechanical-thrombectomy-for-acute-stroke-in-neuro-intervention/
Intracranial Stenting in Neuro Intervention – https://cvicvascular.com/intracranial-stenting-in-neuro-intervention/
AVM Embolization in Neuro Intervention – https://cvicvascular.com/avm-embolization-in-neuro-intervention/