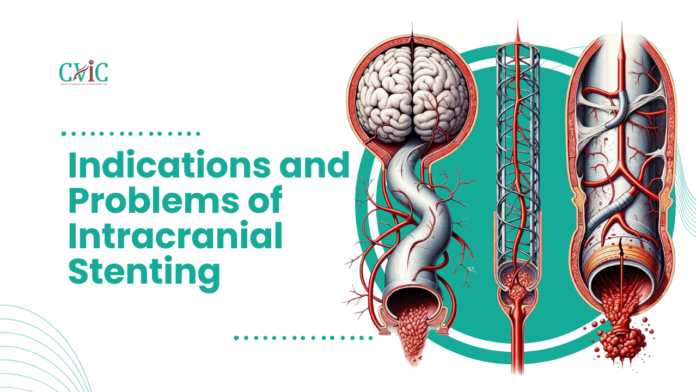
Intracranial Stenting: Understanding the Indications and Addressing the Problems
Intracranial stenting has revolutionized the treatment of cerebrovascular diseases, offering a minimally invasive option to address conditions like stenosis and aneurysms. However, as with any medical procedure, it comes with its own set of indications and potential complications. This article delves into the clinical scenarios where intracranial stenting is considered essential and explores the problems that can arise during and after the procedure.
Intracranial stenting is a medical procedure used to treat certain types of blood vessel problems within the brain. It involves the placement of a small mesh tube, called a stent, inside a blood vessel to keep it open and ensure proper blood flow. This procedure is often used to treat conditions such as:
- Intracranial Atherosclerosis: This is the buildup of fatty deposits and plaque inside the arteries in the brain, which can lead to narrowing (stenosis) and restrict blood flow, increasing the risk of stroke.
- Aneurysms: A stent can be used as part of the treatment for brain aneurysms, which are bulging, weakened areas in the wall of an artery. Stents can help support the artery wall and prevent rupture.
- Vasospasm: Sometimes after a subarachnoid hemorrhage (bleeding in the space surrounding the brain), blood vessels can spasm and narrow. Stents can help keep these vessels open.
Procedure Overview:
- Preparation: The patient is typically given a local anesthetic and a sedative. In some cases, general anesthesia may be used.
- Access: A catheter is inserted into a large artery, often in the groin, and threaded through the blood vessels to the affected area in the brain.
- Placement: Through the catheter, the stent is carefully guided to the site of the blockage or aneurysm. The stent is then expanded to fit snugly against the artery walls, ensuring that the vessel remains open.
- Post-Procedure: The patient is monitored for any complications and may be prescribed medications to prevent blood clots from forming around the stent. Recovery times can vary, but many patients are able to return to normal activities within a few days.
Benefits:
- Improved Blood Flow: The primary benefit of intracranial stenting is to restore and maintain proper blood flow to the brain.
- Stroke Prevention: By addressing narrow or blocked arteries, the risk of stroke is significantly reduced.
- Minimally Invasive: Compared to open surgery, intracranial stenting is less invasive, with shorter recovery times and fewer complications.
Risks:
- Blood Clots: There’s a risk of blood clots forming at the stent site.
- Bleeding: As with any procedure involving blood vessels, there is a risk of bleeding.
- Infection: Though rare, there’s a risk of infection at the catheter insertion site.
- Re-narrowing: In some cases, the artery may narrow again over time.
Intracranial stenting is a specialized procedure typically performed by interventional neuroradiologists or neurosurgeons with expertise in treating complex brain vascular conditions.

Indications for Intracranial Stenting
Treating Intracranial Stenosis
Intracranial stenting is primarily indicated for patients with significant intracranial stenosis, particularly when medical therapy fails to prevent ischemic events. Stenosis refers to the narrowing of the arteries within the brain, which can lead to strokes or transient ischemic attacks (TIAs). When patients continue to experience symptoms despite optimal medical management, stenting can help restore adequate blood flow, thereby reducing the risk of further ischemic events.
Addressing Brain Aneurysms
Another major indication for intracranial stenting is the treatment of brain aneurysms, especially wide-necked aneurysms that are challenging to treat with coiling alone. Stenting helps to support the aneurysm’s neck, allowing coils to be placed more securely within the aneurysm sac. This procedure helps to prevent aneurysm rupture and promotes long-term vessel healing.
Recurrent Stroke Prevention
For patients who have experienced recurrent strokes due to intracranial atherosclerosis, stenting can be a viable preventive measure. It is especially considered when other treatments, such as antiplatelet therapy, have not been effective. The goal is to stabilize the artery and reduce the risk of further stroke incidents by improving blood flow and preventing future blockages.
Resolving Vascular Malformations
Vascular malformations, such as arteriovenous malformations (AVMs), can sometimes be managed with intracranial stenting. By redirecting blood flow away from the abnormal vessels, stenting can reduce the risk of hemorrhage and other complications associated with these malformations. It offers a targeted approach to treating complex vascular conditions within the brain.
Management of Intracranial Dissections
Intracranial dissections, where the inner layers of an artery split and create a false lumen, can also be treated with stenting. This is particularly crucial in preventing the progression of the dissection and the subsequent risk of stroke. Stents help to stabilize the artery walls and restore normal blood flow, preventing further complications.
Problems and Complications of Intracranial Stenting
Intracranial stenting, while beneficial for treating certain vascular conditions in the brain, can present various problems and complications. It’s essential to be aware of these potential issues when considering the procedure. Here are some of the key problems and complications associated with intracranial stenting:
Acute Complications
- Stroke: One of the most significant risks is the possibility of a stroke, either due to the dislodgement of a clot or plaque during the procedure or due to the stent causing a blockage.
- Bleeding: There can be bleeding at the site where the catheter is inserted or within the brain itself.
- Artery Damage: The stent or catheter can sometimes damage the artery, leading to perforation or dissection.
- Allergic Reactions: Some patients may experience allergic reactions to the contrast dye used during the procedure.
Subacute Complications
- In-Stent Thrombosis: Blood clots can form within the stent shortly after the procedure, potentially leading to stroke or other complications.
- Ischemic Events: Reduced blood flow due to clot formation or other issues can cause transient ischemic attacks (TIAs) or strokes.
Long-Term Complications
- In-Stent Restenosis: The artery may narrow again over time due to the growth of scar tissue within the stent, which can reduce blood flow and require additional treatment.
- Stent Migration: Although rare, the stent can sometimes move from its original position, necessitating further intervention.
- Chronic Inflammation: The presence of the stent can sometimes cause chronic inflammation, leading to further complications.
General Complications
- Infection: Infection at the catheter insertion site or within the bloodstream is a potential risk.
- Contrast-Induced Nephropathy: The contrast dye used can affect kidney function, particularly in patients with preexisting kidney conditions.
- Vascular Complications: These can include pseudoaneurysms or arteriovenous fistulas at the catheter insertion site.
Risk Factors
Certain factors can increase the risk of complications, including:
- Patient Age: Older patients may have a higher risk of complications.
- Coexisting Conditions: Conditions like diabetes, high blood pressure, and kidney disease can elevate risks.
- Previous Stroke or TIA: A history of stroke or transient ischemic attacks can increase the likelihood of further ischemic events.
Management and Mitigation
- Pre-Procedural Assessment: Thorough evaluation and preparation can help identify and mitigate risks.
- Antiplatelet Therapy: Medications to prevent blood clot formation are typically prescribed before and after the procedure.
- Careful Monitoring: Close monitoring during and after the procedure can help detect and address complications promptly.
- Follow-Up Care: Regular follow-up appointments are essential to monitor the stent’s condition and overall vascular health.
Intracranial stenting can be a life-saving procedure for many patients, but it’s crucial to weigh the potential benefits against the risks and complications. Discussing these with a healthcare provider can help in making an informed decision.
In-Stent Restenosis
One of the most significant complications of intracranial stenting is in-stent restenosis, where the artery narrows again after stent placement. This can occur due to the growth of tissue within the stent or due to inflammatory responses. Restenosis can lead to recurrent symptoms and may require additional interventions, such as repeat stenting or balloon angioplasty.
Thromboembolic Events
Thromboembolic events are another serious concern, involving the formation of blood clots that can travel and block smaller vessels downstream, leading to strokes. Patients undergoing stenting procedures are typically placed on antiplatelet medications to reduce this risk, but the potential for thromboembolic events remains a significant consideration.
Perforation and Hemorrhage
The risk of vessel perforation and subsequent hemorrhage is a critical complication associated with intracranial stenting. This can occur during the procedure itself or as a delayed complication. Perforation can lead to severe bleeding within the brain, which can be life-threatening and requires immediate medical intervention.
Delayed Aneurysm Rupture
In cases where stents are used to treat aneurysms, there is a risk of delayed aneurysm rupture. Although stents are designed to support the vessel walls and prevent rupture, the manipulation of the aneurysm during the procedure can sometimes weaken the aneurysm sac, leading to a rupture at a later stage.
Infection and Foreign Body Reaction
As with any procedure involving foreign materials, there is a risk of infection and foreign body reaction. Although rare, these complications can lead to serious outcomes if the stent becomes a source of infection or if the body reacts adversely to the stent material. Vigilant post-procedure monitoring is essential to detect and manage such issues early.
Neurological Deficits
Some patients may experience new or worsening neurological deficits following intracranial stenting. These deficits can result from procedure-related complications such as embolic strokes, vessel damage, or hemorrhage. The incidence of such deficits highlights the importance of careful patient selection and meticulous procedural techniques.
Stent Migration
Stent migration, although uncommon, is a potential complication where the stent moves from its original position. This can compromise the treatment efficacy and lead to new vascular complications. Ensuring the correct placement and deployment of the stent during the procedure is crucial to minimize this risk.

Managing and Preventing Complications
Pre-Procedure Planning and Patient Selection
Effective management of complications starts with meticulous pre-procedure planning and patient selection. Not all patients with intracranial vascular conditions are suitable candidates for stenting. A thorough evaluation, including imaging studies and assessment of medical history, helps in identifying patients who are likely to benefit the most from the procedure while minimizing the risk of complications.
Antiplatelet Therapy and Monitoring
Administering antiplatelet therapy before and after the procedure is critical to reduce the risk of thromboembolic events. Monitoring platelet function and adjusting medication as necessary can help in achieving optimal outcomes. Regular follow-up visits are essential to ensure that the antiplatelet regimen is effective and to make any necessary adjustments.
Advanced Imaging Techniques
Utilizing advanced imaging techniques during the procedure can enhance the precision of stent placement and reduce the risk of complications. Techniques such as high-resolution angiography and intravascular ultrasound provide detailed views of the vascular anatomy, allowing for more accurate stent deployment.
Post-Procedure Care and Follow-Up
Post-procedure care is vital in preventing and managing complications. Patients should be closely monitored for any signs of neurological deficits, infection, or other adverse reactions. Follow-up imaging studies are important to assess stent patency and detect any early signs of restenosis or other issues. Timely intervention can prevent complications from becoming severe.
Patient Education and Support
Educating patients about the potential risks and complications associated with intracranial stenting is crucial. Patients should be informed about the signs and symptoms of complications and advised to seek immediate medical attention if they experience any concerning symptoms. Providing support and reassurance can help in managing patient anxiety and ensuring adherence to post-procedure care instructions.
Conclusion
Intracranial stenting offers a promising treatment option for various cerebrovascular conditions, providing a minimally invasive alternative to more traditional surgical approaches. While the procedure has significant benefits, it is not without risks. Understanding the indications for intracranial stenting and being aware of the potential complications can help in optimizing patient outcomes and managing any adverse events effectively.

Frequently Asked Questions
What are the common complications associated with intracranial stenting?
Common complications include in-stent restenosis, thromboembolic events, perforation and hemorrhage, delayed aneurysm rupture, infection, foreign body reaction, neurological deficits, and stent migration.
How can in-stent restenosis be prevented?
Preventing in-stent restenosis involves using antiplatelet therapy, regular monitoring, and potentially utilizing drug-eluting stents that release medication to prevent tissue growth.
What role does patient selection play in the success of intracranial stenting?
Patient selection is critical in ensuring the success of intracranial stenting. Thorough evaluation and careful selection of candidates help in identifying patients who are most likely to benefit from the procedure while minimizing risks.
What should patients expect during the recovery period after intracranial stenting?
Patients should expect close monitoring, regular follow-up visits, and imaging studies to assess stent patency and detect any complications early. They should also adhere to their antiplatelet regimen and be aware of the signs and symptoms of potential complications.
Our Doctors
Dedicated IR Center for Vascular Problems in Madhya Pradesh
DR. SHAILESH GUPTA
MD, PDCC (INTERVENTIONAL RADIOLOGY) Consultant & Co-Director CVIC (Center Of Vascular & Interventional Care)
DR. ALOK KUMAR UDIYA
MD Radiology, PDCC (Neurointervention Radiology), PDCC ( HPB Intervention Radiology) FINR (Switzerland) & EBIR
Endovascular Surgeon & Consultant Interventional Neuroradiologist at Care CHL Hospital, Indore Co-director CVIC( center for vascular and interventional care)
DR. NISHANT BHARGAVA
Consultant Intervention Radiologist
MD Radiology, PDCC ( Neurointervention Radiology), FINR ( Fellowship in Neurointervention Radiology)
Co-director CVIC(Center for Vascular and Interventional Care)
Contact Details
Phone no.
0731 4675670
+91 9827760073
Facebook
https://www.facebook.com/profile.php?id=100092538633553&mibextid=ZbWKwL
Instagram
https://instagram.com/cvic_center?igshid=ZGUzMzM3NWJiOQ==
Google My business
https://g.co/kgs/DrdV3T
YouTube
https://www.youtube.com/channel/UCP5TH5e4iQZkpDUgnLsgZhw
Pinterest
https://pin.it/5DzpX5Z
Twitter
https://x.com/cviccenter?t=01TclSrLFdu0K2re0Gs96w&s=08
LINKEDIN
https://www.linkedin.com/company/center-of-vascular-interventional-care/
Location –
Read More –
How long does it take for kidney to heal after PCNL? – https://cvicvascular.com/how-long-does-it-take-for-kidney-to-heal-after-pcnl/
What is the Success Rate of Tumor Embolization? – https://cvicvascular.com/what-is-the-success-rate-of-tumor-embolization/
What is a Renal Graft Biopsy? – https://cvicvascular.com/what-is-a-renal-graft-biopsy/